Heart disease is a serious thing that can lead to the most common cause of death for both guys and gals. But here’s the deal – heart attacks aren’t always like in the movies, all dramatic and loud. They can sneak up on you suddenly or be quiet, dropping hints a month before the main event. Catching these little signs is essential for a healthy heart journey. Sometimes, the symptoms don’t show up immediately, so it’s like having a secret power to prevent bad stuff.
Get to know these 9 Signs of Heart Attack a Month Before, not just for you but also to be a hero for your friends and family. Stay smart about your heart.
Here are some of the most common signs of a heart attack that you may experience a month before the actual event:
- Frequent Chest Pain
- Fatigue
- Dizziness
- Indigestion or Nausea
- Sweating
- Swelling in the legs, ankles and feet
- Irregular heartbeat
- Pain in other parts of your body
- Shortness of breath

Then we will know the keen details about the signs of heart attack a month before with proof and what research and reports say.
1. Frequent Chest Pain: Major Signs of Heart Attack a Month Before

Chest pain, a major symptom of an impending heart attack, is a critical indicator that should never be ignored. The pain experienced is often described as a pressure or tightness in the chest, resembling the sensation of someone squeezing the chest. This discomfort arises from the compromised blood flow to the heart muscle, leading to distress signals that the body sends out as a warning.
The pain associated with a heart attack is not confined solely to the chest. It can radiate to various body parts, including the arms, neck, jaw, back, or stomach. The nature of the pain, whether sharp or dull and its radiation pattern provide valuable insights into the severity and potential location of the cardiovascular issue.
(#1 USA, UK, Canada) Puravive Customer Reviews: Side effects, Benefits And Huge Discount
Proof:
Numerous medical studies and research, notably from reputable institutions like the American Heart Association (AHA), highlight the robust correlation between chest pain and the occurrence of heart attacks. These studies delve into the physiological mechanisms behind chest pain during a heart attack, emphasizing the role of reduced blood flow to the heart muscle.
American Heart Association’s Research: The AHA consistently underscores the significance of chest pain as a primary symptom of a heart attack. According to their research, chest pain results from ischemia, an inadequate blood supply to the heart. This deprivation of oxygen-rich blood triggers pain receptors, causing the characteristic discomfort associated with a heart attack.
Association with Other Symptoms: The strength of the correlation is further reinforced when chest pain is considered alongside other symptoms commonly associated with heart attacks. Shortness of breath, sweating, and nausea frequently accompany chest pain during a heart attack. This simultaneous occurrence is a crucial diagnostic criterion for healthcare professionals assessing individuals with suspected cardiac issues.
Emergency Room Data: Data from emergency room admissions consistently reflects the prevalence of chest pain among individuals later diagnosed with heart attacks. Emergency room visits for acute chest pain often lead to comprehensive cardiac evaluations, establishing a direct link between the presence of chest pain and the likelihood of a heart attack.
7-Day Kidney Stone Diet Chart: An Essential Nutrition Guide
2. Fatigue: The Early Indicator of Compromised Heart Health

Fatigue, often dismissed as a consequence of a stressful day or restless night, can serve as a subtle yet crucial early indicator of compromised heart health. When experienced disproportionately to one’s usual activities, it may suggest an underlying cardiovascular issue. The relationship between fatigue and the heart’s condition lies in the decreased blood flow to the heart muscle, compelling the heart to work harder than usual. This increased workload can manifest as excessive tiredness.
Understanding the connection between fatigue and compromised heart health involves recognizing the body’s response to circulatory challenges. As blood flow diminishes, the heart’s ability to pump oxygen-rich blood throughout the body is compromised. In response, the heart compensates by exerting more effort, resulting in fatigue beyond the expected tiredness after routine activities.
Proof:
Empirical evidence supporting the link between fatigue and heart attacks, particularly among women, is well-documented in scientific literature. A notable study published in the Journal of the American Heart Association delves into this association, shedding light on the significance of fatigue as a precursor to cardiovascular issues.
Study in the Journal of the American Heart Association: The study, conducted over a significant period, highlights explicitly the correlation between fatigue and the incidence of heart attacks. Researchers observed a higher prevalence of fatigue in individuals who later experienced heart-related events, underscoring its role as a potential warning sign.
Gender-specific Trends: The study’s emphasis on fatigue among women adds a nuanced dimension to its findings. Women, in particular, often experience subtle symptoms before heart attacks, and fatigue emerges as a prominent early indicator. Recognizing these gender-specific trends aids in tailoring preventive measures and health interventions.
Preventive Implications: Understanding fatigue as a precursor provides a valuable window for preventive measures. Individuals experiencing persistent, unexplained fatigue, especially when accompanied by other potential signs of heart issues, should prioritize seeking medical attention. Early intervention can address underlying cardiovascular issues before they escalate into more severe conditions.
What Causes Small Blood Clots in Urine? Unraveling the Mysteries
3. Dizziness: A Pivotal Symptom Signaling Potential Cardiovascular Distress

Dizziness, often attributed to various causes like dehydration or skipping meals, can also serve as a crucial indicator of potential cardiovascular distress. In the context of an impending heart attack, dizziness may arise from inadequate blood flow to the brain. As the heart struggles to maintain proper circulation, insufficient oxygen supply to the brain can lead to lightheadedness or dizziness.
The significance of dizziness is heightened when it occurs in conjunction with other classic heart attack symptoms, such as chest pain or shortness of breath. This combination of symptoms serves as a comprehensive signal of potential cardiovascular issues, prompting individuals to seek urgent medical attention.
Proof:
Scientific research, particularly a study published in the Journal of the American College of Cardiology, substantiates the role of dizziness as a significant symptom occurring before a heart attack. This research contributes to the growing body of evidence linking dizziness to cardiovascular events, emphasizing its importance as a warning sign that should not be overlooked.
Research in the Journal of the American College of Cardiology: The study investigates the correlation between dizziness and the lead-up to heart attacks. By analyzing data from individuals who experienced heart attacks, researchers established dizziness as a prevalent and noteworthy symptom in the prelude to cardiovascular events.
Importance of Recognizing Dizziness: The research underscores the importance of recognizing dizziness as a warning sign for early intervention. Individuals experiencing dizziness, particularly when accompanied by chest pain or shortness of breath, should prioritize seeking medical attention promptly. Acknowledging dizziness as part of a constellation of symptoms helps healthcare professionals make timely and informed decisions in managing potential cardiovascular distress.
Warning: How to Speed Up Nerve Regeneration After Prostate Surgery
4. Indigestion or Nausea: Unmasking Potential Heart Attack Warning Signs

Abdominal discomfort, indigestion, and nausea, typically associated with digestive issues, can also manifest as the body’s response to reduced oxygen in the blood—an ominous precursor to a heart attack. These symptoms may be overlooked due to their seemingly ordinary nature, but they are vital to cardiovascular health.
Reduced oxygen supply to the heart muscle triggers physiological responses, and abdominal symptoms can be a part of this intricate signaling. Acknowledging these symptoms becomes crucial as they can indicate an impending heart attack, warranting prompt attention to prevent further cardiovascular complications.
Proof:
A pivotal piece of evidence supporting the connection between abdominal symptoms and heart attacks is found in a comprehensive study published in Circulation Research. This research underscores the prevalence of abdominal pain in individuals experiencing heart attacks, emphasizing the need to recognize indigestion and nausea as potential warning signs.
Circulation Research Study: The study delves into the intricate relationship between abdominal symptoms and heart attacks. By analyzing data from diverse cases, researchers establish a clear association between abdominal discomfort and cardiovascular events. This association expands understanding of heart attack symptoms beyond the traditional chest pain paradigm.
Importance of Acknowledging Indigestion: The research highlights the importance of acknowledging indigestion as a potential warning sign, urging both healthcare professionals and individuals to consider these symptoms in the broader context of comprehensive health assessments. The findings emphasize that abdominal discomfort should not be dismissed when occurring alongside other potential signs, and further investigation is warranted.
What Is a Transperineal Prostate Biopsy? Revealing the Procedure, Recovery, and Benefits
5. Sweating: Decoding the Stress Response and Its Link to Heart Attacks

Excessive sweating, mainly unrelated to exercise or menopause, indicates the body’s stress response. This physiological reaction is triggered by the activation of the fight-or-flight mechanism, often seen in the context of a compromised heart. Understanding the relationship between sweating and heart attacks involves recognizing the body’s intricate responses to imminent danger.
The body becomes alert when the heart faces challenges due to reduced blood flow or irregular rhythms. This response prompts the release of stress hormones, triggering the autonomic nervous system and leading to profuse sweating. This involuntary reaction signals that the body is under duress and warrants attention.
Proof:
A significant body of evidence supports the correlation between sweating and heart attacks in a study published in the European Heart Journal. This research delves into the physiological mechanisms underlying sweating in the context of cardiovascular events, emphasizing the importance of understanding these responses in recognizing imminent danger.
European Heart Journal Study: The study systematically investigates the association between sweating and heart attacks by analyzing data from individuals who experienced cardiac events. The findings highlight sweating as a prevalent and meaningful symptom, mainly when occurring in conjunction with other indicators of cardiovascular distress.
Physiological Responses and Recognition of Danger: The study emphasizes the correlation and sheds light on the physiological responses leading to sweating. Recognizing these responses becomes crucial in understanding the body’s warning signals and their role in signaling imminent danger related to heart health.
6. Swelling in the Legs, Ankles, and Feet: Unraveling the Significance in Cardiovascular Health
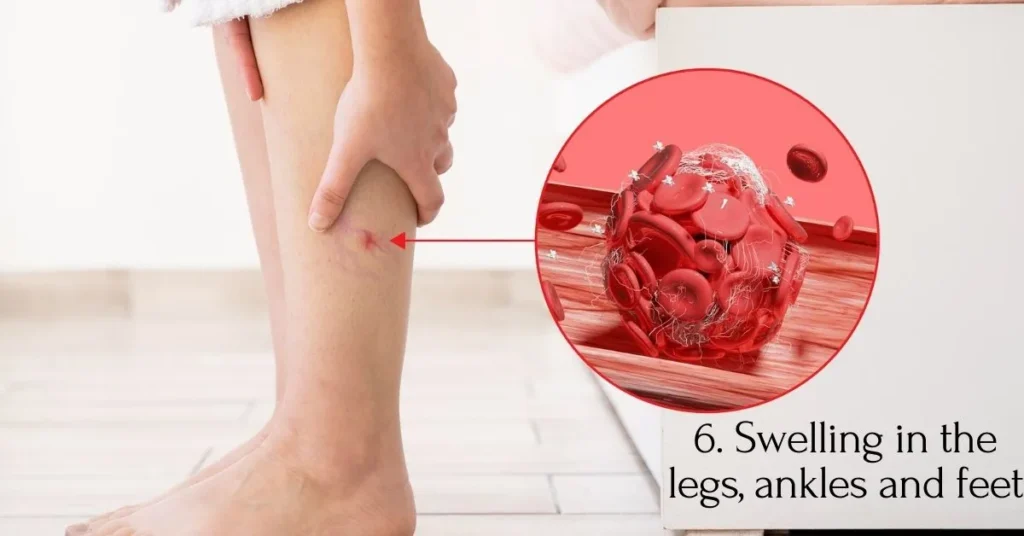
Swelling in the lower extremities, encompassing the legs, ankles, and feet, is a potential red flag indicating inadequate blood circulation—a prevalent issue in the lead-up to a heart attack. This swelling, also known as peripheral edema, may result from compromised cardiovascular function, specifically the heart’s ability to pump blood throughout the body efficiently.
When the heart encounters challenges, such as reduced blood flow or weakened pumping capacity, fluid may accumulate in the extremities, leading to noticeable swelling. Recognizing this symptom is crucial as it can provide valuable insights into circulatory health and be an early warning sign of potential cardiovascular issues.
Proof:
Scientific research, particularly a study in the Journal of Vascular Surgery, sheds light on the connection between swelling in the legs, ankles, and feet and cardiovascular issues. This research contributes to evidence linking peripheral edema to circulatory challenges. It emphasizes the importance of monitoring and recognizing unusual swelling for comprehensive health assessment.
Journal of Vascular Surgery Research: The study explores the relationship between swelling in the lower extremities and cardiovascular health by analyzing data from individuals with documented circulatory issues. The findings establish a clear connection between swelling and cardiovascular challenges, providing a valuable perspective on the role of peripheral edema as a potential indicator.
Monitoring for Unusual Swelling: The research underscores the importance of vigilance in monitoring for unusual swelling, especially in the lower extremities. Recognizing changes in the body, such as persistent swelling, can prompt individuals to seek timely medical evaluation, potentially addressing underlying cardiovascular concerns before they escalate.
7. Irregular Heartbeat: Deciphering an Early Symptom and Its Implications

Atrial fibrillation or irregular heartbeat emerges as an early symptom, significantly impacting the heart’s ability to pump blood efficiently. This condition disrupts the heart’s normal rhythm, leading to irregular contractions of the atria. As a result, the heart may struggle to maintain optimal circulation, potentially posing a risk in the lead-up to a heart attack.
Understanding irregular heartbeat as an early symptom involves recognizing the intricate relationship between cardiac rhythm and efficient blood pumping. An irregular heartbeat can signify underlying cardiovascular issues, and its identification becomes crucial in initiating necessary investigations and interventions to address potential risks.
Proof:
Scientific studies, particularly those published in the Journal of the American Medical Association, establish a robust link between irregular heartbeat and an increased risk of heart attacks. These studies contribute to the growing body of evidence underscoring the significance of recognizing abnormal rhythms as a vital aspect of cardiovascular health assessment.
Journal of the American Medical Association Studies: Research findings reported in the Journal of the American Medical Association delve into the association between irregular heartbeat and heightened heart attack risk. By analyzing data from diverse populations, these studies provide valuable insights into the role of abnormal cardiac rhythms as an early indicator of potential cardiovascular complications.
Recognizing Abnormal Rhythms: The research emphasizes the critical importance of recognizing abnormal heart rhythms as an early symptom. Identifying irregular heartbeat prompts necessary investigations, such as electrocardiograms (ECGs) or Holter monitoring, enabling healthcare professionals to tailor interventions based on an individual’s cardiac profile.
8. Pain in Other Parts of Your Body: Beyond Chest Pain in Recognizing Heart Attack Signs

While chest pain remains a prevalent symptom, it’s crucial to recognize that discomfort in other areas of the body—such as the arms, back, neck, jaw, or stomach—can also be indicative of an impending heart attack. The pain experienced in these regions may vary, presenting as pressure, squeezing, or fullness. Understanding these diverse pain patterns is essential for comprehensive symptom recognition and early intervention.
The manifestation of pain in other parts of the body is not a deviation but a significant variation in how a heart attack can present itself. The interconnected nature of the circulatory system means that compromised heart function can elicit pain signals in areas beyond the chest. Acknowledging these variations contributes to a more nuanced understanding of heart attack symptoms.
Proof:
Scientific research, particularly studies reported in the Journal of Cardiovascular Nursing, delves into the diverse pain patterns associated with heart attacks. This body of evidence emphasizes the importance of understanding these variations in pain presentation to enhance the recognition of symptoms beyond conventional chest pain.
Journal of Cardiovascular Nursing Studies: The studies explore the diverse pain patterns individuals may experience during a heart attack. By analyzing cases and patient reports, researchers establish a clear connection between heart attacks and pain in areas beyond the chest. This insight enriches understanding of the spectrum of symptoms associated with cardiovascular events.
Enhancing Symptom Recognition: The research underscores the significance of recognizing pain in other body parts for accurate and timely diagnosis. Healthcare professionals, armed with a comprehensive understanding of these variations, can tailor assessments to encompass a broader range of symptoms, ensuring that individuals receive appropriate care based on the unique presentation of their symptoms.
9. Shortness of Breath: A Crucial Symptom Indicating Cardiovascular Distress

Shortness of breath, a common symptom, becomes a critical indicator of potential cardiovascular distress associated with inadequate blood flow. The compromised ability of the heart to pump sufficient oxygen-rich blood throughout the body can lead to a sensation of breathlessness. This symptom may occur independently or with other warning signs, such as chest pain, fatigue, dizziness, or nausea.
Understanding shortness of breath due to insufficient oxygen supply underscores its significance in cardiovascular health. This symptom is a physiological response to the heart’s struggle to meet the body’s oxygen demands, and its recognition is vital for prompt medical attention.
Proof:
The American Journal of Emergency Medicine highlights the importance of shortness of breath as a symptom requiring urgent attention. This recognition is substantiated by research findings that emphasize the significance of this symptom in the context of potential cardiovascular complications.
American Journal of Emergency Medicine Findings: The American Journal of Emergency Medicine research emphasizes the significance of shortness of breath as a critical symptom associated with cardiovascular distress. The study underscores the need for timely recognition to facilitate appropriate medical intervention by analyzing cases and outcomes.
Timely Recognition for Appropriate Medical Attention: The research findings stress the urgency of recognizing shortness of breath promptly. When individuals experience this symptom, especially with other potential indicators of heart issues, seeking medical attention promptly becomes paramount. Early intervention can address underlying cardiovascular concerns and prevent the escalation of more severe complications.
Conclusion
Understanding the Signs of Heart Attack a Month Before is pivotal in the journey to heart health. From recognizing frequent chest pain to identifying irregular heartbeats, these diverse warning signals act as life-saving messengers. Whether symptoms manifest suddenly or gradually, their acknowledgment is paramount for timely intervention. By familiarizing ourselves with these indicators, we not only fortify our well-being but also position ourselves as potential lifesavers for those we cherish. Embracing a heart-smart lifestyle and staying vigilant to these signs constitutes a proactive stance, fostering a healthier future for ourselves and our loved ones.
Frequently Asked Questions (FAQ’s)
1. What happens 1 month before a heart attack?
One month before a heart attack, warning signs may include fatigue, shortness of breath, chest discomfort, and unusual fatigue. Risk factors like high blood pressure and cholesterol can contribute. However, symptoms vary, and consulting a healthcare professional is crucial for personalized assessment and preventive measures.
2. What are the early warning signs of a heart attack?
Early warning signs of a heart attack can include chest discomfort or pain, often radiating to the arms, neck, jaw, or back. Shortness of breath, fatigue, nausea, and lightheadedness are also common symptoms. It’s crucial to seek immediate medical attention if experiencing these signs to prevent serious complications.
3. What is 1 rule for surviving a heart attack?
One crucial rule for surviving a heart attack is to seek immediate medical help by calling emergency services (911 in the United States). Time is of the essence, and prompt medical intervention can significantly improve the chances of survival and minimize damage to the heart muscle.
4. What are the symptoms of a mini heart attack?
Symptoms of a mini heart attack, or angina, can include chest discomfort or pain that may feel like pressure, squeezing, or fullness. Pain might also be experienced in the arms, neck, jaw, shoulder, or back. Shortness of breath, fatigue, nausea, and sweating are other possible symptoms. If these signs occur, seeking medical attention is essential.
5. What are the first signs of heart attack in a woman?
The first signs of a heart attack in women can differ from those in men. Common symptoms include chest pain or discomfort, but women may also experience atypical signs such as shortness of breath, nausea, vomiting, back or jaw pain, and extreme fatigue. Recognizing these symptoms is crucial for prompt medical attention.